How a Care Level Assessment Works: A Day in the Life of a German Care Expert
For millions of families, a single home visit can determine access to crucial financial support for care. In Germany, this pivotal role is filled by assessors from the Medical Service (Medizinischer Dienst), who evaluate individuals to assign a Care Level (Pflegegrad). This classification unlocks specific benefits from the statutory long-term care insurance. For American readers, this process is somewhat analogous to the clinical assessments required to qualify for benefits under a private long-term care insurance policy or to determine the level of care covered by certain Medicaid waivers. Join us as we follow Petra, an experienced assessor, on her daily rounds to demystify this critical evaluation and reveal what it takes to qualify for support.
The Assessment Begins: Building Trust and Observing Daily Life
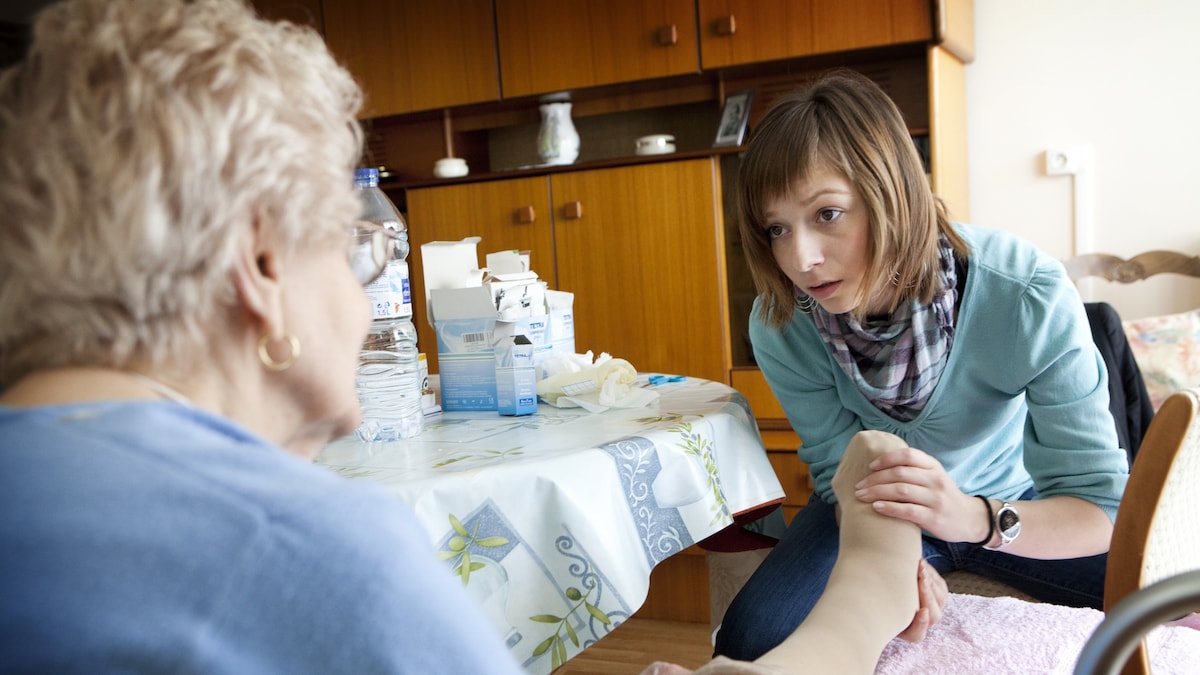
Petra's first visit is to a 90-year-old woman living alone. With no prior information, she enters a new world each time. Her goal is twofold: to provide expert advice and to determine the precise care needs. She starts by building rapport, explaining the process to alleviate pressure. "It's important that people feel comfortable and open up to me," Petra says, as discussions often involve sensitive topics like incontinence or cognitive decline.
The 45-minute assessment is holistic. Petra observes the home environment—checking for loose rugs, bathroom safety, and kitchen accessibility. She reviews medical records, notes height and weight, and inquires about nutrition. But the core of the evaluation lies in observing activities of daily living (ADLs) and instrumental activities of daily living (IADLs).
The "Fist Test" and Reading Between the Lines
A simple request—"Make a fist"—reveals volumes. From this, Petra gauges fine motor skills needed for tasks like buttoning a shirt, brushing hair, or opening a jar. "You develop an eye for it," she notes. In this case, the woman's numbness and inability to manage zippers or peel an apple point to significant decline. Despite her insistence on independence, her constant use of a personal emergency alarm speaks to underlying insecurity. Petra reads these subtle cues "between the lines."
Her conclusion: Care Level 2 (Pflegegrad 2), denoting "considerable impairments." This qualifies the woman for a monthly relief allowance of €131 and, crucially, a care cash benefit of €347 if cared for by family, or higher-value benefits for professional in-home care services.
Beyond Physical Health: The Cognitive Assessment
The next visit is to a 78-year-old man with prostate cancer. While physical tests like raising his arms are telling, the conversation takes a turn when his partner mentions, "He forgets a lot." Petra shifts focus, asking specific cognitive questions:
- "What is your address?" (Spatial orientation)
- "What day is it today?" (Temporal orientation)
- "What did you have for lunch?" (Short-term memory)
His delayed responses and need for prompts indicate cognitive challenges separate from his cancer. Petra recognizes that the primary need stems from emerging dementia, not the oncology diagnosis. Again, she assigns Care Level 2, accounting for both his mild physical and now-evident cognitive restrictions.
The High Stakes: What Different Care Levels Mean for Benefits
The assessor's judgment directly translates into financial support. The difference between levels is substantial. Here’s a simplified breakdown of key benefits at the lower levels:
| Care Level (Pflegegrad) | General Description | Monthly Relief Allowance | Cash Benefit for Family Care | Benefit for Professional Care (Sachleistung) |
|---|---|---|---|---|
| Care Level 1 | Minor impairments, largely independent. | €131 | €0 | ~€42 (for care aids) |
| Care Level 2 | Considerable impairments. | €131 | €347 | Up to €796 |
As seen, the jump from Level 1 to Level 2 significantly increases support, especially for accessing professional care services. A single point in the assessment can influence this classification.
A U.S. Perspective: Contrasting Evaluation Systems
While Germany uses a standardized national assessment for a public insurance fund, the U.S. approach is more fragmented:
- Private Long-Term Care Insurance: Evaluations are conducted by assessors appointed by the insurance company, similar to Petra's role, but criteria and benefits vary wildly by policy.
- Medicaid: State-conducted assessments determine eligibility for programs like Home and Community-Based Services (HCBS) waivers. These often have strict financial and functional ("nursing home level of care") criteria, which can be more restrictive than Germany's five-tier system.
- Common Thread: Both systems rely heavily on evaluating ADLs (bathing, dressing, toileting, transferring, continence, feeding) and cognitive status to gauge need.
The Assessor's Challenge: Empathy, Objectivity, and Detecting Fraud
Petra's job requires a delicate balance. She must connect empathetically with individuals sharing stories of trauma or depression while remaining objectively focused on measurable impairments. "We assess the limitation, not the illness," she states. She is also vigilant for potential fraud, estimating she detects inconsistencies in 95% of cases. "It's social benefits money," she explains. "We must ensure it's used where truly needed." This was clear in a third visit, where she denied a requested upgrade for a man with addiction and lung disease because his functional abilities had not declined.
Key Takeaways for Families Navigating Care Needs
Whether you're in Germany facing a Pflegegrad assessment or in the U.S. applying for long-term care insurance benefits or Medicaid, preparation is key:
- Document Everything: Have medical records, a list of medications, and a diary of daily challenges ready.
- Be Open and Detailed: Don't minimize struggles. Explain what a "bad day" looks like. Show the assessor the unopened jars or the unused stove.
- Understand the Criteria: Familiarize yourself with the evaluation domains (mobility, cognition, self-care, etc.). In the U.S., know your insurance policy's or state's specific "benefit triggers."
- Seek Advocacy: Consider having a family member, social worker, or patient advocate present during assessments to ensure all concerns are communicated.
The work of assessors like Petra highlights the complex, human-centered process behind care funding decisions. As populations age on both sides of the Atlantic, understanding these systems is the first step toward securing the necessary support for dignified aging. Proactive long-term care planning, including understanding assessment processes, is essential for every family's future security.